Outstanding IT Software at the 2026 TITAN Business Awards - Read More
AI in Healthcare: Use Cases, Benefits & Implementation
For healthcare organizations evaluating AI adoption, the decision isn’t about whether the technology works but about choosing the right implementation path. Below we break down proven real-world applications, the operational and financial returns providers are already seeing, and a scalable integration framework built for measurable business impact.
Written By:

VP – Digital Marketing
Expert Insights By:

VP – Ops & Delivery
- $187.95B
- Market by 2030
- 37%
- Annual Growth rate
- $200B+
- Annual Savings with AI
- 147%
- ROI in 3 Years
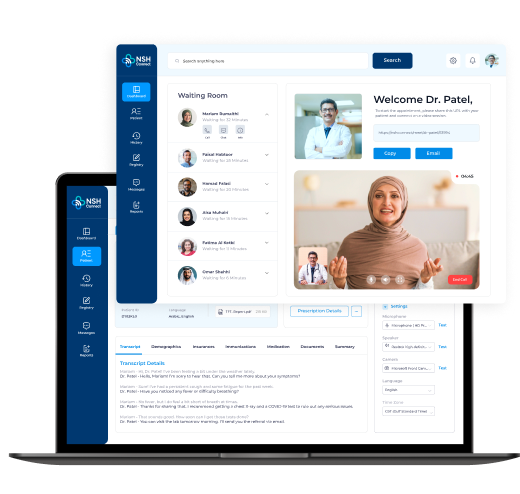
AI in healthcare is the technology layer that converts clinical data, operational workflows, and patient behavior into decisions that improve margins, reduce errors, and drive competitive advantage across the care continuum. AI in healthcare uses intelligent algorithms to analyze patient data, automate clinical workflows, and surface insights that improve both care quality and operational efficiency. It operates across diagnostics, surgery, drug discovery, remote monitoring, and revenue cycle management. Providers using it are cutting costs, reducing errors, and making faster decisions with greater confidence. The case for adoption is no longer theoretical. Health systems with the right integration strategy in place are already measuring the returns others are still projecting.
How AI Differs from Traditional Healthcare IT
| Feature | Traditional Healthcare IT | AI in Healthcare |
|---|---|---|
 Logic Model Logic Model | Rule-based and strictly deterministic. | Adaptive, probabilistic, and self-learning. |
 Data Interaction Data Interaction | Manages and organizes structured data. | Interprets structured and unstructured data. |
 Primary Goal Primary Goal | Streamlining administrative documentation. | Enhancing clinical and diagnostic accuracy. |
 Outcome Nature Outcome Nature | Static; the system follows instructions. | Dynamic; the system improves with more data. |
 Example Example | Electronic Health Record (EHR) storage. | Predictive analytics for patient risk levels. |
 User Role User Role | Human interprets all data provided. | AI surfaces insights for human validation. |
How AI is Transforming Healthcare?
The healthcare industry is undergoing a radical shift, driven by a need to move from reactive treatments to proactive, data-driven wellness. Artificial Intelligence is the critical engine addressing these core market pressures.
Data Explosion in Healthcare
Health systems drowning in EHR, wearable, and genomic data cannot afford manual processing. AI converts that volume into clinical decisions that protect revenue and patient outcomes simultaneously.
Demand for Precision Medicine
Generic treatment protocols cost providers in readmissions and adverse outcomes. AI delivers patient specific therapy recommendations that improve efficacy, reduce liability, and position your practice as a precision care leader.
Operational Inefficiencies
Clinician burnout and administrative bloat are revenue problems before they are culture problems. AI automates scheduling, billing, and patient flow so your workforce performs at capacity without the overhead.
Regulatory Pressure
Compliance failures are expensive. AI driven documentation and real time data monitoring keep healthcare organizations audit ready, reducing the financial and reputational risk of human error across every reporting requirement.
Shift Toward Value-Based Care
Value based contracts reward outcomes, not volume. AI tracks long term patient health, prevents costly readmissions, and aligns your operational performance directly with the reimbursement models replacing fee for service.
The State of Artificial intelligence in Healthcare Industry
AI in healthcare has moved decisively from pilots and experimentations to enterprise-scale adoption. Healthcare providers are increasingly embedding ML and Gen AI applications into core systems for AI-assisted radiology, clinical decision support, fraud detection and hospital workflow optimization.
Regulatory pressure, operational costs, clinician shortages, and patient data volumes are increasing the need for secure, compliant AI infrastructure.
“AI has shortened wait times in my practice by reducing image review time from 48 hours to under 6 hours for eye scans... but setup costs are expensive for small practices, ranging from $18,000 to $40,000 per workstation"

Dr. Rron Bejtullahu
Challenges in Implementing AI in Healthcare

Data Privacy & HIPAA Compliance
Protecting sensitive patient information is the cornerstone of healthcare trust. AI systems require access to vast amounts of Protected Health Information (PHI) to function effectively, which inherently increases the surface area for potential cyber threats and unauthorized data leaks.
For us, maintaining rigorous HIPAA compliance and international standards like GDPR is non-negotiable. That’s why we implement robust end-to-end encryption, de-identification protocols, and strict access controls to ensure that innovation never comes at the cost of patient confidentiality or legal standing.

Integration with Legacy Systems
Many healthcare providers still rely on aging infrastructure and fragmented "siloed" databases designed decades ago. These legacy systems often lack the modern APIs or processing power required to feed data into sophisticated AI models, creating a significant technical bottleneck for real-time analysis.
We bridge this gap by using a middleware strategy or comprehensive cloud migration. Success depends on creating a unified architecture where AI can coexist with existing Electronic Health Records (EHRs) without disrupting clinical workflows or causing system downtime.

Data Quality & Interoperability
AI is only as good as the data it consumes, yet healthcare data is notoriously messy. Information is often trapped in inconsistent formats across different departments—ranging from handwritten notes to various imaging standards—which prevents a cohesive "single source of truth" for the algorithm.
We avoid that by standardizing this data through frameworks like FHIR (Fast Healthcare Interoperability Resources) and ensuring seamless exchange. Without high-quality, normalized data, AI outputs remain unreliable, leading to "garbage in, garbage out" scenarios that can compromise decision-making.

Model Bias & Validation
If an AI model is trained on non-representative datasets, it can inadvertently inherit and amplify human biases. This leads to skewed diagnostic or treatment recommendations that may negatively impact specific demographic groups, raising serious ethical and clinical concerns regarding the fairness of the technology.
We, at Radixweb, thus emphasis continuous clinical validation and "algorithmic auditing" to ensure accuracy. Our AI healthcare software developers prioritize diversity in training data and maintain transparency in how models reach conclusions to build the necessary "explainability" that clinicians and regulators demand.

Change Management & Training
The most advanced technology will fail if the human workforce is not prepared to use it. Many clinicians view AI with skepticism, fearing it may replace their expertise or add more "screen time" to an already over-burdened schedule, leading to significant resistance during the rollout phase.
For effective implementation, we recommend building a culture of continuous learning and clear communication. We help organizations invest in comprehensive training programs that demonstrate AI as a supportive "co-pilot" rather than a replacement. With that, we ensure that your staff feels empowered and competent in the new digital landscape.
Real-World AI Use Cases: From Theory to Clinical Impact
At Radixweb, we view AI not as a standalone product, but as a strategic layer that amplifies medical expertise. The following use cases of artificial intelligence represent the current frontier of healthcare transformation, where data matures into life-saving intelligence.
Predictive Analytics for Patient Outcomes
Predictive modeling transforms reactive care into a proactive shield. By synthesizing longitudinal patient records, real-time vitals, and socioeconomic factors, AI identifies high-risk individuals long before a clinical crisis occurs. This foresight allows providers to intervene during the "golden window," significantly reducing hospital readmissions and preventing the escalation of chronic conditions.
Implementation in Action:
Penn Medicine successfully deployed a predictive AI system known as Penn Signals. By analyzing real-time data from Electronic Health Records, the system identifies patients at risk of sepsis or heart failure up to 30 hours in advance. This early warning gives clinical teams the lead time necessary to adjust treatment protocols, which has measurably improved survival rates within their intensive care units.
Automated Radiology & Imaging Analysis
Radiology is currently facing a massive data bottleneck, with imaging volumes far outstripping the number of available specialists. AI-driven computer vision acts as a "force multiplier," pre-screening thousands of scans to highlight subtle anomalies (such as micro-calcifications or early-stage nodules) that might be invisible to the fatigued human eye. This ensures that the most critical cases move to the top of the radiologist's queue instantly.
Implementation in Action:
Mayo Clinic has integrated AI algorithms directly into their neurology workflows to assist in the analysis of brain MRIs. The AI specifically targets the detection of stroke symptoms and traumatic brain injuries, flagging urgent scans for immediate review. By automating the preliminary screening process, they have significantly reduced the "door-to-needle" time for stroke patients, where every second saved preserves millions of brain cells.
Clinical Decision Support Systems (CDSS)
Modern CDSS acts as a cognitive co-pilot for clinicians. It filters through vast medical libraries, latest research papers, and patient-specific data to provide evidence-based treatment recommendations. This reduces the cognitive load on doctors and minimizes the risk of human error, ensuring that every patient benefits from the collective global knowledge of the medical community.
Implementation in Action:
Memorial Sloan Kettering Cancer Center (MSK) has long been a pioneer in using advanced computational systems to assist oncologists. Their implementation focuses on matching a patient's specific genetic profile with the most effective chemotherapy or clinical trial options. By processing millions of pages of medical literature, the system provides doctors with a ranked list of treatment pathways tailored to the individual’s unique tumor markers.
Intelligent Hospital Workflow Automation
The operational "backbone" of a hospital is often its biggest source of friction. AI optimizes the logistical dance of healthcare—from predicting peak ER arrival times to automating nurse shift scheduling and bed management. By treating the hospital as a dynamic ecosystem, AI ensures that resources are always where they are needed most, eliminating the "wait-and-see" approach to facility management.
Implementation in Action:
The Johns Hopkins Hospital utilizes a sophisticated "Capacity Command Center". This AI-driven hub uses predictive screening to manage patient flow across the entire facility. It predicts bed shortages before they happen and coordinates transfers between departments. Since its launch, the hospital has seen a 60% improvement in its ability to accept patients with complex conditions from other regional hospitals.
Fraud Detection & Revenue Cycle Optimization
In the complex world of medical billing, errors and fraudulent claims cost the industry billions annually. AI analyzes billing patterns in real-time to identify "upcoding," duplicate claims, or suspicious billing spikes. Beyond security, it optimizes the revenue cycle by predicting which claims are likely to be denied, allowing administrative teams to correct documentation before submission.
Implementation in Action:
UnitedHealth Group employs deep learning models to scan hundreds of millions of claims for irregularities. Their AI systems can differentiate between simple clerical errors and sophisticated fraudulent schemes with high precision. This proactive detection not only saves the organization billions in potential losses but also streamlines the reimbursement process for legitimate providers by reducing the need for manual audits.
Virtual Patient Assistants & Chatbots
AI-powered conversation assistants serve as the first point of contact, providing 24/7 triaging and health guidance. Unlike basic automated menus, these intelligent agents use Natural Language Processing (NLP) to understand patient intent, assess symptom severity, and direct individuals to the appropriate level of care. Whether it's a home remedy or an immediate ER visit.
Implementation in Action:
Northwell Health implemented a specialized AI "chatbot" to stay connected with patients after they leave the hospital, particularly for those undergoing high-risk procedures like colonoscopies. The assistant sends automated, conversational check-ins to monitor recovery and answer preparation questions. This has resulted in a higher patient engagement and a significant reduction in "no-show" appointments for critical follow-ups.
Personalized Treatment & Therapy Planning
AI moves healthcare away from "standardized" protocols toward "individualized" cures. By analyzing a patient’s unique phenotypic and genotypic data, AI helps oncologists and specialists craft therapy plans that are biologically optimized for that specific person. This is particularly transformative in oncology and rare disease management, where the difference between a "standard" and "custom" dose can be life-altering.
Implementation in Action:
Intermountain Health uses AI to power its precision medicine program, specifically for late-stage cancer patients. Their system analyzes the genomic sequence of a patient’s tumor to identify specific mutations that might respond to targeted therapies. This approach has allowed them to provide personalized drug recommendations that have, in many cases, improved the progression-free survival time compared to traditional "one-size-fits-all" chemotherapy.
RPM & Wearable Analytics
The hospital of the future is the patient's home. AI-driven RPM platforms ingest a continuous stream of data from wearables like heart rate, oxygen levels, glucose, and sleep patterns. The AI acts as a "digital sentry," alerting care teams only when the data indicates a trend toward instability, allowing for remote interventions that prevent emergency hospitalizations.
Implementation in Action:
Mount Sinai Health System utilizes AI-driven RPM to manage patients with chronic conditions like hypertension and diabetes. Patients use connected devices at home, and the AI analyzes the daily readings. If a patient’s blood pressure trends upward over three days, the system automatically alerts a care coordinator to adjust the medication remotely. This program has successfully reduced ER visits among chronic disease population.
Bring The Use Cases To Life, With Experts
Speak to our strategists and implement AI in your workflows today
The Technological Engines of Modern Healthcare
Machine Learning Models
Machine Learning forms the analytical core of healthcare AI. These models ingest historical patient data to identify hidden correlations, allowing systems to predict disease onset or medication responses with high precision. It is the foundation for truly personalized, data-driven medicine.
Natural Language Processing (NLP)
NLP acts as the bridge between human language and digital intelligence. By analyzing unstructured clinical notes, discharge summaries, and research papers, NLP extracts vital data points that would otherwise remain trapped in text, significantly accelerating clinical documentation and patient history reviews.
Computer Vision
Computer Vision transforms medical imaging into a high-speed diagnostic tool. By training on millions of radiological images, these algorithms detect minute anomalies in X-rays, MRIs, and CT scans faster than the human eye, ensuring that life-critical findings are never overlooked or delayed.
Predictive Analytics
Predictive Analytics shifts the healthcare paradigm from reactive to proactive care. By processing real-time vitals and historical trends, it forecasts potential health crises—such as sepsis or cardiac events—allowing clinical teams to intervene early, improve survival rates, and drastically reduce hospital readmissions.
AI Agents for Workflow Automation
AI Agents are autonomous digital coworkers designed to handle complex, multi-step administrative tasks. From coordinating staff schedules to managing bed availability in real-time, these agents eliminate operational friction, allowing medical professionals to dedicate their full attention to patient interaction and care.
Generative AI in Clinical Documentation
Generative AI is revolutionizing the "clerical" side of medicine by auto-synthesizing patient-doctor conversations into structured medical records. This technology drastically reduces the time spent on EHR entry, directly combating clinician burnout and ensuring more accurate, comprehensive, and timely clinical documentation.
Benefits of AI in Healthcare
Operational Benefits
Reduced Administrative Workload
AI acts as a digital force multiplier by automating the high-volume, repetitive tasks that typically consume a clinician's day. By utilizing Natural Language Processing (NLP) for medical transcription and automated coding for billing, healthcare organizations can drastically cut down on manual data entry. This shift not only minimizes human error in documentation but also directly combats provider burnout by allowing medical staff to return their focus to face-to-face patient care.
Faster Diagnosis
In critical care, time is the most valuable asset. AI accelerates the diagnostic pipeline by instantly pre-screening diagnostic data—such as blood work or medical imagery—to flag urgent abnormalities for immediate physician review. By reducing the "wait time" between a test and its interpretation, AI ensures that life-saving treatments are initiated hours or even days earlier than traditional manual workflows would allow.
Improved Workflow Efficiency
AI transforms hospital logistics from a reactive struggle into a streamlined, predictive operation. By analyzing historical patient flow and real-time bed occupancy, machine learning models can forecast peak admission periods and optimize staff scheduling accordingly. This ensures that resources—from nursing shifts to operating room availability—are always aligned with actual patient demand, eliminating bottlenecks and reducing overall wait times.
Clinical Benefits
Better Patient Outcomes
The ultimate benchmark of healthcare AI is its ability to improve the quality of life and recovery rates. By providing continuous monitoring and real-time clinical alerts, AI systems ensure that subtle physiological declines are caught before they escalate into emergencies. This constant "digital oversight" results in lower mortality rates, fewer post-surgical complications, and a more robust recovery process for patients across all departments.
Personalized Treatment Plans
Moving away from the "average patient" model, AI leverages genomic data and lifestyle analytics to tailor medical interventions to the individual. These systems analyze how a specific person’s biological makeup will likely respond to various medications, allowing doctors to prescribe the most effective drug at the optimal dosage from the start. This precision medicine approach maximizes therapeutic impact while significantly reducing the risk of adverse drug reactions.
Early Disease Detection
AI excels at identifying "the invisible," catching the earliest markers of chronic conditions like cancer or cardiovascular disease long before they are symptomatic. Through advanced pattern recognition in imaging and pathology, AI can detect cellular changes that the human eye might miss. Catching these conditions in Stage 0 or 1 fundamentally changes the prognosis, often turning a life-threatening diagnosis into a highly manageable or curable one.
Financial Benefits
Cost Reduction
While the initial investment in AI is significant, the long-term ROI is driven by massive gains in operational economy. By preventing expensive hospital readmissions, reducing the length of patient stays through better care coordination, and eliminating waste in the supply chain, AI helps healthcare systems operate at a much lower cost-per-patient. Automation of back-office functions further slashes overhead, protecting the organization’s bottom line.
Risk Mitigation
AI serves as a sophisticated safety net that identifies potential clinical and financial risks in real-time. Whether it is flagging a potential drug-to-drug interaction before a prescription is filled or identifying a fraudulent billing claim before it is submitted, AI reduces the likelihood of costly legal liabilities and regulatory fines. This proactive approach to risk management ensures that the organization remains compliant and reputable in a highly scrutinized industry.
Competitive Advantage
In an increasingly digital-first market, AI-enabled healthcare providers stand out as leaders in innovation and patient safety. Adopting AI allows organizations to participate in lucrative value-based care contracts that reward high-quality outcomes over volume. Furthermore, the ability to offer cutting-edge, personalized care helps attract both elite medical talent and a tech-savvy patient base that prioritizes efficiency and advanced treatment options.
Leverage AI to optimize workflows and patient outcomes.
Enterprise Security & Compliance Framework for Healthcare AI Systems
Regulatory Standards & Industry Compliance Alignment
FDA & Software as a Medical Device (SaMD)
AI algorithms used for diagnosis or treatment planning often fall under SaMD regulations. We align development with FDA Quality System Regulations (QSR), focusing on rigorous clinical validation and pre-market notifications. By maintaining a clear "audit trail" of model training and testing, we help organizations navigate the complex path to regulatory approval for medical-grade AI.
Security Best Practices for Healthcare AI Infrastructure
AI Governance, Risk Management & Operational Oversight
Model Explainability & "Black Box" Reduction
For a doctor to trust an AI, they must understand why a recommendation was made. Our healthcare data governance framework prioritizes "Explainable AI" (XAI) techniques, providing clinicians with heatmaps or feature-importance scores that highlight the data points influencing a diagnosis. This transparency transforms the AI from an opaque "black box" into a verifiable clinical partner.
Future Trends of AI in Healthcare
The trajectory of healthcare AI is moving from "experimental" to "infrastructural." AI-models like ChatGPT and Claude have launched specialized healthcare offerings. We are seeing a shift where AI is no longer a bolt-on feature but the very core of how health systems operate, driven by a global market projected to reach $505 billion by 2033 and 90+% adoption rates.
AI-Powered Precision Medicine
Precision medicine is evolving from a niche genomic research tool into a mainstream clinical reality. By 2026, AI is being used to synthesize "multi-omics" data (combining genomics, lifestyle, and environmental factors) to create hyper-individualized treatment pathways.
The Trend: Moving away from "one-size-fits-all" to "n-of-1" medicine where treatments are unique to a single patient’s biology.
The Data: The AI in Precision Medicine market is expected to grow at a CAGR of 34.33% through 2035, with AI in oncology leading the charge with a 31% market share.
Autonomous AI Agents in Hospitals
The era of simple chatbots is over; 2026 marks the rise of "Agentic AI"—autonomous digital entities that don't just answer questions but execute complex workflows. These agents act as "clinical wingmen," managing everything from patient intake and real-time triaging to automated billing and follow-up care without human intervention.
The Trend: Autonomous agents performing multi-step tasks like predicting sepsis and immediately triggering diagnostic protocols.
The Data: By the end of 2025, 94% of healthcare leaders already expected AI agents to be essential across their operations to combat a clinician burnout rate that currently affects over 50% of providers.
Real-Time Clinical Intelligence
Clinical intelligence is shifting from retrospective reporting to live, bedside decision support. In 2026, "Ambient AI" is the standard in exam rooms, listening to patient-doctor conversations and auto-generating structured clinical notes with higher accuracy than human-written reports.
The Trend: Live integration of AI into the EHR (Electronic Health Record) to provide instant "alternative point of view" second opinions for complex diagnoses.
The Data: AI-generated surgical notes currently show an accuracy of 71%, significantly outperforming the 53% accuracy found in traditional surgeon-written documentation.
AI-Driven Population Health Management
Health systems are now using AI to manage the health of entire communities rather than just the patients inside their walls. By analyzing social determinants of health (SDOH) and data from the Internet of Medical Things (IoMT), AI predicts which populations are at risk for chronic outbreaks or rising readmission rates.
The Trend: Predictive analytics enabling a "proactive" rather than reactive healthcare model, focusing on wellness and early intervention.
The Data: AI-driven predictive models have demonstrated the potential to reduce hospital readmission rates by up to ~15% and lower mortality rates by 30%.
Generative AI in Drug Discovery
By 2026, Generative AI has moved from text generation to "molecule generation." Pharmaceutical companies are using GenAI to simulate drug effects and run virtual clinical trials, which drastically slashes the traditional 10-year development cycle.
The Trend: Shortening drug development timelines from years to months and reducing R&D costs by repurposing existing drugs for new, off-label uses.
The Data: Experts predict that AI-driven drug repurposing will slash R&D costs by 25% by the end of 2026, making treatments for rare diseases more financially viable.
Read more about other latest healthcare technology trends here.
Radixweb’s Specialized AI Healthcare Portfolio
At Radixweb, we don’t believe in "plug-and-play" AI. We engineer bespoke, medical-grade intelligence that integrates deeply with your existing clinical and operational DNA.
AI-Driven Clinical Decision Support Systems
We build cognitive co-pilots that combine patient history, real-time vitals, and clinical research to provide evidence-based guidance at the point of care. These systems help physicians make faster, more accurate decisions while maintaining transparency through explainable AI.
- Real-time clinical decision intelligence
- Evidence-based treatment recommendations
- Reduced diagnostic variability across teams
- Transparent and explainable AI insights
- Faster decision-making at point-of-care
Predictive Patient Outcome Analytics
Our predictive AI and ML models transform healthcare data engineering by helping healthcare providers identify high-risk patients before conditions escalate. By analyzing historical and real-time health data, these systems enable proactive care interventions that improve outcomes and reduce emergency treatment costs.
- Predicts readmissions and disease escalation
- Identifies high-risk patient populations
- Enables proactive clinical intervention
- Improves long-term patient outcomes
- Reduces emergency care costs
Medical Imaging & Diagnostic Intelligence
We use advanced computer vision to automate and accelerate medical imaging analysis. These systems help detect anomalies earlier and prioritize critical scans for faster specialist review.
- AI-powered medical image analysis
- Detects subtle diagnostic anomalies
- Prioritizes high-risk imaging cases
- Improves diagnostic consistency and speed
- Reduces radiologist workload significantly
Intelligent Hospital Workflow Automation
Our AI solutions streamline hospital operations by automating administrative workflows and optimizing resource allocation. This ensures smoother patient flow and improved operational efficiency across healthcare facilities.
- Optimizes hospital resource allocation
- Predicts peak patient arrival patterns
- Automates staffing and scheduling workflows
- Reduces administrative operational friction
- Improves patient flow across departments
Healthcare Fraud Detection & Revenue Cycle AI
We build AI models that safeguard healthcare revenue cycles by detecting billing anomalies and fraudulent claims. These systems also improve billing accuracy and minimize costly claim denials.
- Detects billing anomalies and fraud
- Flags duplicate and uncoded claims
- Predicts claim denial risks
- Improves billing efficiency and accuracy
- Protects healthcare revenue integrity
AI-Powered Patient Engagement & Virtual Assistants
Our AI-powered virtual assistants help healthcare providers deliver continuous patient support through automated triage, scheduling, and care guidance.
- 24/7 AI patient assistance
- Automated triage and appointment scheduling
- Personalized patient health guidance
- Improves medication adherence rates
- Reduces front-desk operational workload
What Makes Radixweb a Trusted AI Healthcare Software Development Company?
With 25+ years of engineering excellence, Radixweb bridges the gap between complex AI innovation and the rigorous demands of the medical industry. We don't just build healthcare software solutions we build compliant, life-saving digital ecosystems.
Deep Domain & Compliance Expertise
We navigate the complexities of HIPAA, GDPR, and FDA regulations as a core part of our development DNA. Our ISO 27001:2022 certification ensures that every AI model we deploy meets the highest global standards for data security and patient privacy.
Interoperability-First Approach
We specialize in breaking down medical data silos. By utilizing FHIR/HL7 standards and secure API layers, we ensure your AI solutions communicate seamlessly with legacy EHRs, imaging systems (PACS), and lab databases for a unified "single source of truth."
Proven Clinical Value Delivery
Our focus is on "Actionable Intelligence" rather than just data. From reducing clinician burnout with ambient AI to improving patient outcomes through predictive analytics, our solutions are benchmarked against real-world clinical KPIs and ROI.
Real-World Impact: Our Success Stories
Frequently Asked Questions
What is AI in Healthcare?
What is the cost of AI healthcare software development?
What is the timeline for AI healthcare software development?
How do you handle security and compliance for AI in healthcare?
What is the AI healthcare software development process?
Schedule A 1-on-1 AI Strategy Session
Speak to our experts and find out
Step 1: Fill in the form & share your requirements
Step 2: Sign an NDA, if needed to ensure 100% privacy
Step 3: Get on a call with our AI experts and get a practical understanding of cost, timeline, and ROI.
Business Inquiry
Tell Us About Your Project for Tailored Guidance
By submitting this form, you agree to our Privacy Policy